Noon Report: Calciphylaxis
/Hospitalist 2 team presented an excellent noon report this week on diagnosing a patient with new onset calciphylaxis in an ESRD patient. Here is a quick review of calciphylaxis:
Calciphylaxis is a disease characterized by occlusion of microvessels in subcutaneous adipose tissue and dermis that results in painful, ischemic lesions. Risk factors for the disease include ESRD, obesity, female sex, diabetes, hypercalcemia, hyperphosphatemia, and vitamin K deficiency. Caliphylaxis can be classified as nonuremic or uremic. Nonuremic cases are often associated with medications (warfarin, recombinant PTH) and primary hyperparathyroidism. Uremic, cases in patients with ESRD, are the most common. The initial skin lesions may include induration, plaques, nodules, livedo, or purpura. They frequently progress to develop netlike areas of erythema with rapid progression to malodorous ulcers with black eschars. Cause of death is most commonly sepsis from secondary wound infection.
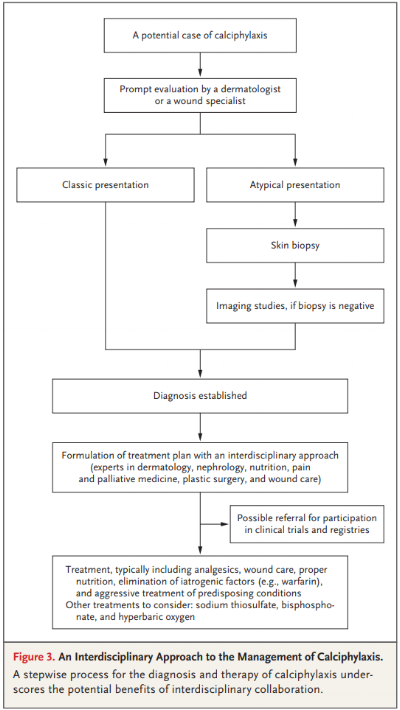
Pathogenesis of calciphylaxis is unclear but research has shown an impaired inhibition of calcium phosphate precipitation. Elevation of serum calcium and phosphate levels are non-specific for diagnosis but commonly seen. Skin biopsy is the gold standard for confirmation of diagnosis however, its role is debated given the risk of provoking new ulcers. A biopsy is not needed for patients with ESRD and a classic presentation. Biopsy should be considered if a patient presents atypically or if calciphylaxis is suspected in non-ESRD patient.
Treatment of calciphylaxis includes pain control, discontinuing iatrogenic causes including warfarin, and decreasing elevated Ca and PO4 levels. Hemodialysis frequency and duration is often increased. Sodium thiosulfate, which inhibits adipocyte calcification and prevents calcification of vascular smooth muscle, is often used for treatment but data is limited. Vitamin K supplementation has also shown beneficial results in select studies.
Check out a review article from NEJM here
Authored by: GREGORY WIGGER, MD